You are currently browsing the tag archive for the ‘labor’ tag.
Dear Andrea,
You don’t know me, but you know my parents. All I know about you is that my parents are fond of you. You work at a coffee shop that my parents frequent. Your baby girl was born yesterday…Congratulations!
My mom was anxiously awaiting the news of your girl’s birth just like she was waiting for news of my baby boy’s birth just 12 weeks ago. Last evening, mom shared with me that you went into labor at 2 AM and that you started pushing at 6:30 PM. After 2 hours of pushing, mom was waiting for imminent news! After 3 hours of pushing, she shared that you needed a c-section.
I want to write you because your story struck a very familiar chord with me. I want to put this on my blog because I know I’m actually writing to a lot more women than just you!
My baby will be 3 months old in one week…which means I’m almost 3 months removed from all the very raw emotions surrounding my baby’s birth. I’m nearly 3 months into my physical healing. I can tell you that three months out is a really good place to be!
I don’t know you, Andrea. I don’t know anything of your hopes and dreams for your baby’s birth. I don’t pretend to know what you are feeling right now. I only know how I felt at the time of my baby’s birth.
Then, I was disappointed that I couldn’t push my baby out on my own– after ~19 hours of labor with ~4 1/2 hours of pushing. I needed help via an episiotomy, which made me feel like a failure. I didn’t have a c-section like you did, but it’s only because I’d labored so long at a birth center first. My midwife literally gave it all she had before she transferred me to the hospital. Had I been in the hospital to start with, I would have had a c-section for certain.
At the time, I thought to myself, “Thank God it’s over and he’s out and I didn’t have a c-section!” At the time, I thought that a c-section was the worst case scenario. But why? A scar? Painful healing? Healing that takes longer than a vaginal birth?
Hmm…
My healing from childbirth has made me re-think all of that. Is a c-section really “so” bad? I don’t know. But I can tell you that healing from my vaginal birth has included 1) a scar, 2) painful healing and 3) a long time frame for healing– exactly those things that I feared with a c-section.
Sure, I don’t have an abdominal scar. But I still have a belly that shows that I’ve carried a baby. As I lose the fat underneath my skin, the skin is still looser than it was before. It may tighten up over time, but I suspect that it won’t ever be like it was before I had my baby. And I’ve decided that’s okay! I wouldn’t trade my baby for my pre-pregnancy belly.
Second, my healing process has been very painful! It’s taken a LONG time to simply feel normal again. Seriously, it’s just been in the past week that I’ve felt significantly better. The pressure in my perineum when I walk and shop and carry my baby and move his carseat with him in it is so much less.
My point is: no matter what kind of birth you have, it may take a long time to feel good again. My intention is not to scare you but to reassure you. I caused myself undue stress by assuming that I would heal a lot quicker than I did. I thought 6 weeks would be the very longest it would take me to feel good again. Oh, NO! Not even close. I sincerely hope you heal faster than I have, but if you don’t, please don’t worry! Give yourself time. The waiting really really sucks, but it will happen! Make patience your best friend.
When I was in the midst of physically feeling really, really bad, week after week after week, I had a lot of time to think about all the “what ifs”:
- What if I’d had a c-section? Would I have had less pain? Would I have healed faster? Is that possible?
- What if I’d started out in the hospital to begin with? Would my baby have needed the NICU if I hadn’t pushed for those extra hours? (**See note.)
- What if my baby didn’t go to the NICU? Would I have been successful with breastfeeding?
- What if I’d had an epidural instead of doing it unmedicated? Would I have been less physically spent when he was finally born? Would I have been able to feel elation when he came out instead of feeling dazed and traumatized?
- What if I’d been able to birth my baby vaginally without an episiotomy cut? How much different would I feel?
- What if I hadn’t taken castor oil to induce me at 41 weeks + 2 days? Would I have gone into labor on my own before 42 weeks anyway? Would I have had an easier labor? Would it have changed the outcome?
What if, what if, what if? Why do we do that to ourselves? Yep– if I’d had a c-section, you can bet that I’d be playing the same “what if” game from that perspective. It’s insane!!
What points am I trying to make? What advice do I want to give?
When we’re pregnant, it’s only natural that we want the perfect birth experience. When that happens it’s great! I’m sooo happy for those lucky ladies! But if it didn’t happen for you, then try to be gentle with yourself. It’s not your fault. You did the best you could. Give yourself the time to grieve for the birth experience that you wanted but didn’t get. Give yourself a lot of time. Time does heal. Know that the post-partum hormonal crash makes every sad feeling feel so much worse.
Nope– I’ll never know if changing one or more variables in my labor and delivery experience would have turned my traumatic experience into a satisfying one. With every passing month, I’m letting go of the what ifs. I’m getting closer and closer to…acceptance.
Yep– now that I’ve had my own “less-than-ideal childbirth and failed breastfeeding” experiences, I realize that my thinking on this topic is no longer “black and white” like it used to be.
Before, it was a little too easy to assume that a hospital birth would be bad and a birth center birth would be good…an epidural would be bad, and an unmedicated birth would be good…a c-section would be bad, and a vaginal birth would be good…formula feeding would be bad and breastfeeding would be good…etc, etc.
Now I know that there’s plenty of good and bad in all of it. A lot of things are out of our control, anyway.
Andrea– congratulations again! Enjoy your new baby girl. Rest when you can (easier said than done, I know!) Recover. Accept help whenever you can. Do what’s best for you and your baby. These next few weeks will probably be difficult, but you’ll get through it. The learning curve can be rough, but pretty soon you and your baby will have a “flow.” Enjoy each phase of your newborn’s development. It’s true that they grow so fast! I’m starting to have a lot of fun with my almost 3 month old.
Sincerely,
Elisa
(P.S.: I’m still a brand new mom!)
————————————–
(**Note that my baby was never in any distress while I was pushing. I do not fault my midwife in any way whatsoever. I support her and all of her decision making surrounding my labor. And, during my 6 week post-partum check-up we actually had this same “what if” conversation.)
Click here to read my baby’s birth story.
As I complete this post, it’s now September 18, 2014, and my #minivegan is 4 weeks old. This story of Todd’s birth is quite long, but I didn’t want to leave anything out…
Before I detail how Todd’s birth day actually played out, I feel the need to outline what I’d hoped for in a birth experience:
I planned to deliver Todd in the birth center where I’d been receiving all my prenatal care. My midwife, doula, husband, sister, and 10 year old niece would be present. I expected labor to be difficult, painful work, but not anything that I couldn’t handle. I was strangely, honestly never fearful or anxious leading up to the onset of labor. I wanted to experience it fully without any medication that would dull the sensations. I wanted to have pictures and maybe video footage of Todd when he emerged from my body.
I pictured my husband perhaps catching him, and Todd being brought up to my chest immediately after. His cord clamping would be delayed. I would enjoy the flood of oxytocin and the “high” that I’d read about, immediately after his arrival. Breastfeeding would be initiated as soon as possible. Later, we would all enjoy the quiet time together. Finally, we would share the birthday cake that we made for the occasion.
——————————————————-
And here’s what REALLY happened. As “they” say, things don’t always turn out according to plan…
As per the recommendation from my midwife on Wednesday, August 20th, I ingested 2 ounces of castor oil at bedtime that night. It was about 9:30 or 10 PM. I drank it plain. It was quite thick and somewhat tasteless. “Let the games begin,” I wrote on Facebook. Famous last words!!
The midwife told me to expect contractions to come ~2 minutes apart right away due to the castor oil, so I should not be surprised about that.
Something made me wake up at about 11:30 PM. I didn’t get back to sleep after that, so I got only 1.5 hours of sleep to prepare me for the next ~19.5 hours…
Oddly, I don’t remember when the contractions started. I also don’t remember when the horrendous watery diarrhea started. I do know that I was back and forth from my bed to the bathroom many times in those early hours. It was bad enough to make me really NOT want to repeat the 2 ounce caster oil dose again at 2 AM, like I was instructed to do.
Just before 2 AM, I called the midwife’s pager, seeking advice regarding the castor oil. Ultimately, I followed my gut and I didn’t repeat the dose. I’m sure glad about that!
I started timing contractions at 2 AM, using a phone app. For about an hour, they were lasting about 45 seconds to 1 minute duration, coming 2-2.5 minutes apart, and they were of “moderate” severity.
At about 3 AM, I started rating my contractions at “strong” intensity. Duration = ~1 minute. Frequency= every 2-3 minutes, with a few longer breaks. I felt the worst pain as a “ring of burning” around my hips.
I called my doula (Serena) at 3:15 AM to tell her that I needed her. She arrived at 3:50 AM. I don’t know when the vomiting started, but I sure had poor Eric cleaning up my bathroom. Serena wrote in her notes that I had “lots of puke” before her arrival, and that my last vomit was at 5 AM.
From the time she arrived, Serena would press in firmly against my hips to try and ease the intense burning pain around my hips.
At 4:20 AM, I had some leaking fluids that we suspected was my “water” breaking. It wasn’t a big gush. While at home, I labored on my bed, using the birth ball, leaning over the kitchen sink, sidelying on the floor, and sidelying on the couch. Serena suggested I try to walk a little outside, but I just could not do it. No way. Too bad, because the weather was clear and it was probably a nice morning for a walk.
At 6:20 AM, Serena thought it was time to call the midwife and go to the birth center. Jane was the midwife on call. I was glad it was her, because I’d seen her the most during my pregnancy. But I would have been happy if Brianna took the call, too. They are both great!
At 7:00 AM, we arrived at the birth center. In order to make the short walk to/from the car more bearable, Serena wrapped a long piece of fabric tightly around my hips to provide compression.
At 8:00 AM, I got my first dose of Penicillin, since I was GBS+.
At 8:45 AM, I was dilated to 5 cm, and Jane opened my cervix up to 7 cm.
At 9:00 AM, I got into the tub. I stayed there for a long time because I felt the best there.
At 10:00 AM, my sister went to the store to get me some Coconut Bliss ice cream. Unfortunately, I ate very little that day, but the ice cream was soothing and provided me with needed calories.
Earlier, I had some watermelon and a cherry flavored soy yogurt. In retrospect, I should have been eating a lot more. I took in fluids regularly while in the tub, but I’m sure I was still quite dehydrated from the early morning diarrhea. Later on in the afternoon, I don’t remember drinking much.
At 12:20 PM, Jane did a cervical check, and I was at 9 cm. I forced the smile in the picture below. It was possibly the only time I smiled that day. In the tub, I remember thinking to myself repeatedly that it’s a good thing I’m only going to do this once. The pain was The Worst Ever. I tried so hard to simply breathe through it, but sometimes it was just too unbearable and I would vocalize a sort of moan or a cry. But, for what it was, I think I did a good job handling it.
At 2 PM, I started pushing while in the tub.
(By the way– I was not really aware of time throughout the whole labor. I have recreated the exact timeline from the notes I received from Serena and Jane, along with date stamps on our photos and videos.)
I started out pushing while leaning back against the tub. A half hour later, I pushed on a birth stool in the tub. I felt inside myself and I could feel baby’s head. I was encouraged.
At some point when I was on the birth stool, Jane had to do something REALLY, SUPER, PAINFUL. She said that baby was not advancing over a 1/2 cm anterior cervix lip. She had to stretch and manipulate my cervix during the pushes, in order to get baby’s head to move past the barrier.
I have 3 video clips of that part. It must have taken 3 contractions for Jane and I to accomplish it, because the video clips are about 3 minutes apart. When I watch and listen, I get tense and I can feel my heart rate increase. O-M-G. That’s a pain I’ll never forget.
Pushing was very frustrating to me. I never really had the urge to push. It was hard for me to tell when to start and when to stop. I remember mentioning this to Jane several times. I needed her guidance constantly. I tried to breathe through the pushes and to avoid holding my breath. Nothing about this phase felt instinctual.
At 3 PM, I tried pushing from reclining on the bed. At some point, I was instructed to sit on the toilet to push. Jane was having me try all different positions.
At 3:15 PM, I pushed on the birth stool with a Rebozo (a ~5 ft long Mexican shawl) wrapped around my back (held by Serena), while my legs were braced up against Jane’s chest.
All this time, baby’s heart rate was staying in the 120s-140s. I don’t remember when it was that Jane mentioned something about baby “not tucking his head.” Was that what was taking so long? He was doing a brow presentation?
At 4 PM, I was instructed to assume all fours on the bed, with my head and arms down on pillows and my butt up in the air. I remember being left alone for some time, and I felt really lost. I still couldn’t tell when the contractions started and stopped. I still wasn’t feeling urges to push. Later on, I would learn that this position was used for the purpose of trying to reposition the baby somehow, so that he would advance better.
It must have been around this time that my family was getting concerned. For myself, I was definitely “checking out” more and more. I stopped opening my eyes. I was getting more and more fatigued from the unending pain and exertion. At some point, I remember asking, “What time is it, anyway?” I don’t remember what the answer was.
At 4:25 PM, I was due for another dose of Penicillin. I was also given IV fluids (sodium chloride). Then, I was back on my back with legs drawn up. I would continue to push that way for another 2+ hours.
Jane and Serena kept telling me that I was really effective with my pushes, but baby would go back up between each contraction. After a while, I started to wonder if they were just being encouraging. (When I met with Serena days after the birth, she told me that they were being encouraging, but it was also true. That made me feel a little better.)
At 5:50 PM, baby’s head was crowning. Jane said that I needed to deliver soon. I had to find more strength with each push. I heard the urgency. I especially heard it in my sister’s voice when she pleaded, “c’mon, c’mon.” I heard the worry and the desperation in her voice. It makes me emotional to think about it. I started holding my breath and bearing down hard with everything I had. (This caused lots of burst blood vessels in my face, especially around my eyes.)
At the time, I thought I was “so” close, but looking back, I really don’t think I was. Jane wrote in her notes that 4 cm of baby’s head was visible in the last hour. She tried to help stretch my perineum as I pushed: more excruciating pain. It wasn’t enough. Through all of this, baby’s heart rate remained in the 130s.
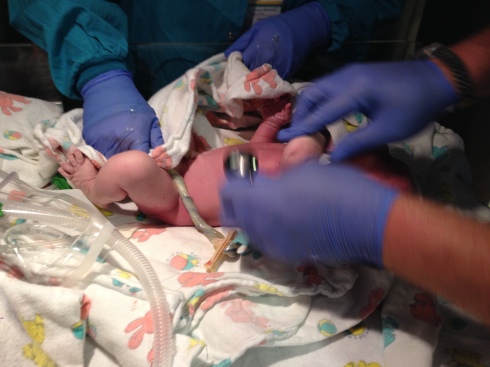
After 6:30 PM, I was completely exhausted, both mentally and physically. It was clear to all that I needed some extra help. Jane said baby needed a vacuum extraction. I had to be transferred to the hospital, at Providence, which was a few blocks away.
The ambulance was called. I heard the sirens. Eric said they used a full sized fire truck to block off Colby street. I hadn’t opened my eyes in a couple hours and I never opened them while I was being moved from bed to gurney. I never looked at the EMS personnel who helped me. I don’t know what it looked like inside the ambulance. All I remember were the voices and the sound of my now continuous moaning. They put an oxygen mask on my face and they started an IV line in my arm. I reached down and I could feel baby’s protruding head.
Eric, meanwhile, got our things packed up in the car, and he ran lights to try to catch up to the ambulance. He didn’t know where to go, exactly. (We never took a hospital tour!) Fortunately, he managed to get there right when they were loading me into the elevator. He asked if he could come into that elevator, but they said he should wait. He told them, “That’s my wife,” and then they let him in.
My sister and niece drove separately. Unfortunately, they first went to the wrong Providence campus, which is located further north in Everett, before being directed back to the correct location. I guess Ashley cried during my ambulance transfer. It makes me sad to think about it. I’m sorry she had to see me having so much difficulty. I didn’t see them until later.
Once I got into the hospital room, I finally opened my eyes. I swear I remember someone telling me that they were giving me some Fentanyl. I had IV lines in both arms. Later, I would ask about that. Oddly, there was no documentation that I ever got Fentanyl. Weird. My memory of that is so vivid. I don’t think I would have been given that drug in the ambulance. (??)
The doctor said she would do an episiotomy, so she would give me a local anesthetic. When she warned that it would hurt a little, I actually laughed a little to myself. What’s a little pain from a needle poke after what I’d been through?! Eric told me later that it was a nurse who suggested the episiotomy. Once the cut was made, I was ready to push during the next contraction. At this point I still doubted my ability to get baby out. I still feared a C-section. I gave that push everything I had left.
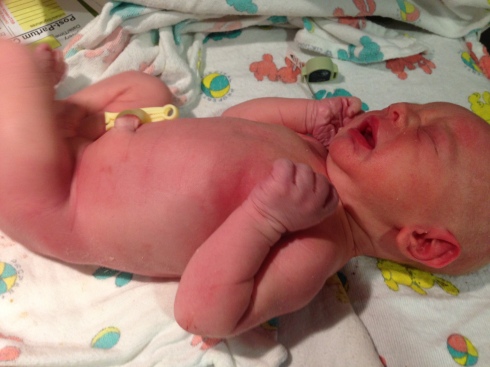
It was 7:08 PM, and baby Todd came right out. Eric said the doctor reached both hands in there and guided him out. I saw my baby boy for the first time just briefly as the medical personnel quickly lifted him up and moved him to a bassinet near the foot of my bed. He didn’t come right to my chest. There was no delayed cord clamping. But oddly, I just did not care. My overwhelming feeling was just the immense relief that he was out. And it was over. And he looked healthy. And it was over. I could finally relax.
Video of Todd at 7:15 PM: IMG_1742
Video of Todd at 7:44 PM:
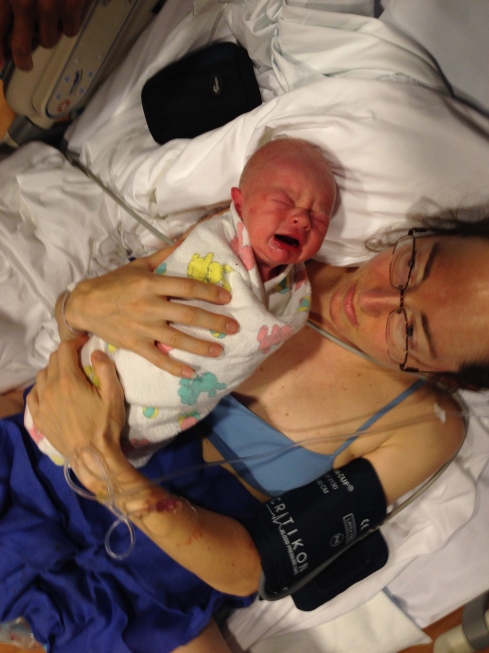
At 7:45 PM, the nurse brought Todd to me for the first time. I was still pretty dazed, though. It was awkward to hold him because the IV in my right elbow crease prevented me from bending my arm enough. That was annoying. But it felt really good to have him in my arms.
After the birth, Serena and Jane were allowed to visit me. Serena brought me some pop and pretzels (the only vegan snack options she could find in the hospital at the time). Jane took the pictures of me holding Todd for the first time:
The whole time that Todd was away from me and being manipulated by the medical staff, Eric was with him. Eric had noticed some twitching that became a concern because of the possibility of seizure activity. Because of that and because of an elevated white blood cell count, they wanted Todd to go to the NICU. They wanted to give him IV antibiotics as a precaution against infection. Another disappointment.
My sister and niece came into the room to visit me after Todd was sent to the NICU. It was a great comfort to see them. My sister said she was so sorry about all that I went through. It wasn’t the joyous birth experience we’d all hoped for, with all of us together. Of course, the important thing was that Todd appeared healthy.
When Ashley tried to visit Todd in the NICU, she was denied access because of her age. To know that happened and that she cried over not being able to finally see baby Todd just broke my heart. That sweet girl had been anticipating Todd’s arrival more than anyone else, and she was with me the whole day. It was so upsetting. She had to wait a full 24 hours before she could finally meet him and hold him, because that’s how long Todd was in the NICU.
I was transferred to a different hospital room, and I went to visit Todd in the NICU a little while later. Eric slept in my room overnight, and we visited Todd again the next morning, at about 7:30 AM. Eric went home for a while.
I visited Todd in the NICU every few hours that day. He made cute frog noises, so Eric gave him the nickname, “Ribbit.” The neonatologist decided during their staff rounds in the late morning that Todd didn’t need any more IV antibiotics. There was no concern about seizure activity. The only thing that kept him in the NICU longer was maintaining his blood sugars.
Video of Todd at 2:53 PM on 8/22/13:
In the late evening, Todd was discharged from the NICU and brought to my room. Ashley finally got to meet him and hold him. I was sooooo happy!! We stayed one more night in the hospital.
On Saturday, August 23rd, we got to go home!
Reflecting back, 4 weeks later–
I know it sounds really bad, but initially I considered my baby’s birth day to be the worst day of my life. Why? It was not just the physical pain. If that was the only thing, then it would have been okay. Even though it was the very worst pain ever, I do feel like I coped with it well. What made it bad was the pain compounded by everything else:
- feeling like a failure because I couldn’t get my baby out on my own
- having to be transferred to the hospital
- not having my family present at the end (other than Eric)
- being unable to feel intense joy once he came out (because I was utterly spent)
- being personally separated from my baby in the minutes/hours/day after birth
- not having intimate family time with Todd after his birth
Of course, what made it the worst day wasn’t “that” he was born, it was “how” he was born. I’ve done a lot of crying. I’ve had to process my sadness and my disappointment. I wanted it to be different. I know I should count my blessings. It could have been worse in a thousand ways. I am grateful. But it’s still normal to grieve, and I’ve had to do a lot of that. It hasn’t been easy. I’m only human.
Writing this post (and others to come) is one way that I can give some closure to the experience. I love my baby Todd so very much. I’m so glad he was born. But I’m so glad that I don’t ever have to go through childbirth again. Maybe it would be different and better “next time,” but we are definitely “one and done.”